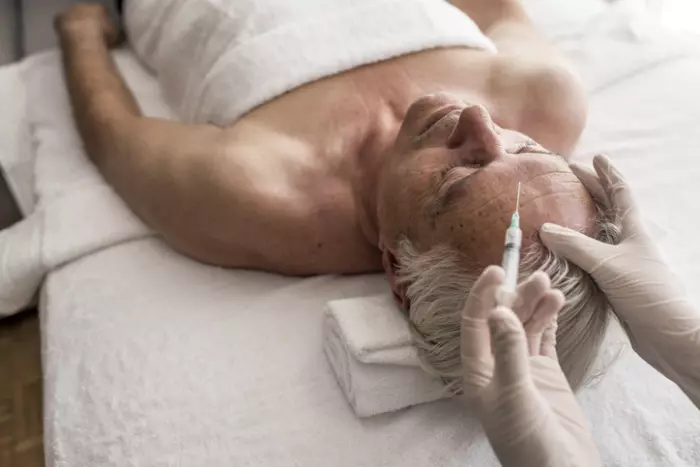
If you want to know what makes Marie Guerin feel queasy, show her a YouTube video of an American influencer injecting fillers into her own face.
“She’s injecting so close to her eye she could easily blind herself,” says Guerin, a registered nurse and owner of Wellington’s Accent on Skin.
It’s what can happen when the cosmetic appearance industry is unregulated, she says.
Guerin, who’s been involved in the sector for 25 years, became so concerned about the lack of regulations and standards that she helped to set up the Cosmetic Appearance Nurses Network of New Zealand for nurses who inject Botox and dermal fillers. She and a fellow nurse also recently established a training school for practitioners to provide a more formalised pathway to gaining experience and training.
Some context: Botox is a toxin made by the bacterium Clostridium botulinum which freezes muscles to stop creases and wrinkles caused by facial expressions (typically found in the upper face, such as the forehead and around the eyes). Dermal fillers, on the other hand, are sometimes called soft tissue fillers and are designed to be injected beneath the surface of the skin to add volume and fullness.
 Marie Guerin. Photo: Supplied.
Marie Guerin. Photo: Supplied.
Evidence shows that the number of unqualified people taking these procedures – and needles –into their own hands has leapfrogged in the past few years, thanks to the industry being left largely to regulate itself.
But in the United Kingdom, the authorities are fighting back: in May, Parliament there passed the Botulinum Toxin and Cosmetic Fillers (Children) Act, which bans under-18s from undergoing cosmetic procedures such as Botox and fillers. Figures show that a whopping 83% of treatments there involving injectables were performed by people without medical qualifications and training, from beauticians and hairdressers to those operating out of their kitchens.
“The UK used to be the wild west as far as our industry is concerned,” says Dr. Catherine Stone, owner of Auckland’s The Face Place. “But with the passing of this act, they’re now better regulated than us.”
The first doctor in New Zealand to specialise full-time in cosmetic injections, Stone says New Zealand currently has no age limit on treatments.
“It’s up to the discretion of the provider. I would never inject anyone under 18, but having said that, in my career I have injected a two-year-old with cerebral palsy when I worked in hospitals, and also a couple of 14-year-olds for excessive sweating. But those were for medical reasons, which are vastly different to cosmetic reasons.”
The waters have been further muddied by the fact that a decade or so ago, dermal fillers in New Zealand were moved from the prescription medicine register and reclassified as a medical device.
“What this means is that while Botox is still a medicine that can only be administered by qualified medical personnel such as doctors, nurses and dentists, dermal fillers can be bought and used by anyone,” says Stone.
Guerin says that in New Zealand, “the only regulator is the companies who sell fillers, and while they are ethical and don’t sell to those they don’t think are qualified, there’s nothing to stop people buying them from overseas on the internet”. That means, as Stone puts it, that “Fred from down the road can inject people from his house”.
There’s also the issue of some clinics, particularly those driven by profit rather than results, seemingly adding to the problem, says Guerin. “Some of these clinics bring in self-employed contractors, and if someone asks a contractor for bigger lips – even though they know it’s not aesthetically or morally right, but they have to pay their mortgage that week – what are they going to do?”
 Dr. Catherine Stone. Photo: Supplied.
Dr. Catherine Stone. Photo: Supplied.
It can be difficult to understand how widespread this issue is, given this country has no official statistics on how many New Zealanders are getting Botox or fillers, or how much the industry here is worth.
Hans Raetz, president of the New Zealand Society of Cosmetic Medicine, told Stuff that “appearance medicine is an entirely ‘private’ speciality with no involvement of the official health-care bodies”.
“This makes securing statistics rather difficult,” he says. “If you want an educated guess as to what we believe to be the current trend in New Zealand, Botox used to be by far the most common treatment, and while that’s increasing year on year, fillers are quickly catching up."
The problem is that unqualified operators don’t have the knowledge, experience, or emergency equipment if things go wrong.
“Our clinic has equipment such as defibrillators and medicine to reverse any adverse reactions,” says Guerin. “We can recognise things like a blocked blood vessel and know what to do about it.”
Both Botox and dermal fillers are considered safe, but as with any medical procedure, there’s always a risk that something will go wrong.
“The biggest issue with filler is a vascular occlusion, or a blocked blood vessel,” says Stone. “Registered medical experts have Hyalase on hand, an enzyme that can dissolve the filler if this happens and fix the blockage.”
Filler administered in the wrong place can also cause blindness, which has happened once in New Zealand. Less severely, it can also result in unsightly lumps and nodules, swelling, scarring and necrosis, a form of cell injury that results in the premature death of cells.
Both Stone and Guerin are often the ambulance at the bottom of the cliff when such procedures go wrong. “It comes in waves, but sometimes we’ll see a couple of patients a week who come to us to fix treatments they’ve had elsewhere,” says Stone.
The most common issues are over-filled lips – the so-called “duck pout” – but she also puts right botched procedures such as puffiness under the eyes and over-filled cheeks.
One of the main reasons for the increase in the use of injectables is social media, where celebrities and influencers often flaunt their cosmetic procedures.
“Social media has normalised over-filled treatments,” says Stone. “Look at the Kardashians and others who promote over-filled lips, plus people like Kylie Jenner who create an unrealistic aesthetic for young age groups. The fastest-growing sector of our industry is 20- to 30-year-olds, whereas our core clients used to be 35- to 55-year-olds.”
Over-the-top treatments aren’t, however, high on the list of requests for Stone or Guerin. “Our patients are interested in the natural look,” says Stone. “A high proportion come from the corporate world and they want subtle changes to facial wrinkles that will make them look less tired, stressed and grumpy. Many still want to be perceived as competitive among a younger workforce, especially in industries which do not always celebrate the wisdom that age brings.”
While there’s currently no sign that New Zealand is following the UK’s regulatory example, the Ministry of Health reports it is continuing work on the draft therapeutic products bill. Introduced in 2019, the bill seeks to bring greater regulation into the cosmetic medicine industry. Both the Society of Cosmetic Medicine and the Cosmetic Appearance Nurses Network made submissions on the bill, seeking tighter laws regulating who can and can’t administer dermal fillers.
“I’m not sure why the bill hasn’t been introduced into Parliament yet,” says Guerin, while Stone takes it a step further: “Perhaps the government see us a frivolous industry and don’t take us seriously. But something has to be done and I hope it doesn’t take a serious event before there’s change.”
Any change needs to include ensuring that those administering dermal fillers are well qualified and part of a registered group.
“They also need to be regularly audited to ensure they know what they’re doing and have the right training and emergency equipment should something go wrong,” says Guerin.
Stone says fillers also need to go back onto the prescription medicine register to ensure that only doctors, nurses and dentists can administer them. “And no more being able to buy them from the internet!”