My previous article highlighted that using the Canterbury model of devolving responsibility through subsidiarity should be the primary focus. But there is so much more that can be done.
First and foremost, we need to rekindle and enable innovation.
The 1990s saw huge technological innovation in New Zealand healthcare and by 2000 we were the envy of the world. Since then, innovation has stalled and, disappointingly, we have fallen behind other countries.
How did this happen? Well, the answer is bureaucrats grabbed hold of the innovation steering wheel.
Administrative hurdles were introduced and the modest amounts of discretionary funding for doctors to develop new solutions dried up. Centrally controlled "innovation hubs" were set up that mostly delivered nothing. While the intent was good, formalised or centralised innovation is an oxymoron.
Health information technology (IT) innovation still has flickers of life but is mostly moribund. Even after numerous Ministry of Health-authored IT vision documents and plans, little has happened. We continue to spend so much to get so little. The solution is multifaceted, but it is definitely NOT a bigger Wellington-based health IT operation.
Some people suggested we buy a big monolithic American IT system, which is an absolutely dumb idea on many counts.
These heinously expensive systems, originally designed for the US insurance healthcare system, are a poor fit for NZ. Often, they deliver little or no value for US hospitals and they would extinguish any remnants of homegrown Kiwi innovation.
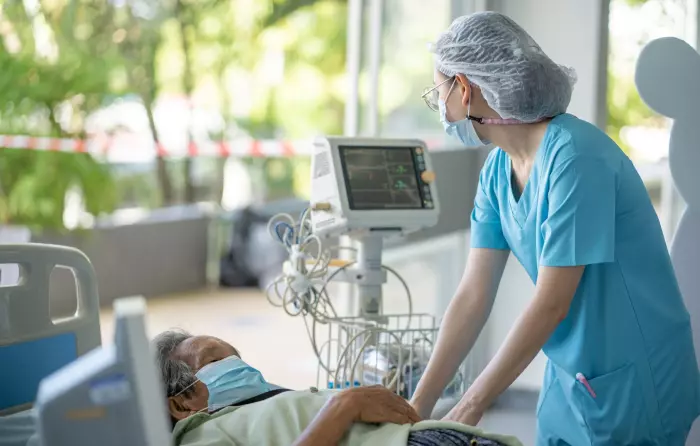
Make frontline health a priority
The solution to getting NZ healthcare back to the top of the class is to return to frontline clinical staff having modest funding to solve real local problems. The goal would then be to roll out successful solutions across the country.
Frontline health workers and their innovative thinking are the key to unlocking our woes. Not more Wellington boffinry.
In addition, the government's addiction to consultants needs to end as they seem to be giving rubbish advice (like centralising decision-making), are self-serving and bloody expensive.
The 2022 spend on consultants by the Ministry of Health ballooned to $154 million from an already eye-watering $63 million the previous year. Furthermore, the government should be asking for a refund of some of the $30m spent on a health reforms plan, which wasn’t finished.
Enough savings here would pay for a few thousand nurses, midwives, etc, and I am pretty sure we all agree that is what we need the most.
NZ has a huge healthcare worker shortage that needs addressing. Our 2020 health workforce was 253,000, including a reported 22% shortfall in senior medical officers. So, probably 50-60,000 new staff are needed.
This is an impossible task when battling the headwinds of retirements (50% of GPs will retire over the next 10 years), very low training rates by OECD standards, poor working conditions, burnout, understaffing (GPs on average look after 1,500 patients when the ideal number is ~1,000), and other countries aggressively targeting our health professionals offering a lot more money.
Even if we fixed recruitment processes, we’re unlikely to even get close to recruiting the numbers needed or being able to afford the extra salaries.
A big to-do list
Fortunately, subsidiarity healthcare devolves a considerable amount of work to community health workers and primary care staff, thereby freeing up the likes of specialists, hospital beds and ED capacity for more acute patients.
Furthermore, the post-Canterbury earthquake experience shows devolved healthcare delivers a whole lot more healthcare with the same resources.
Tens of millions could also be saved by fixing procurement. As I have publicly stated before, our health procurement processes are amateurish, lack accountability, are sometimes dishonest and much more.
They are some of the worst in the developed world, which I can authoritatively say as Orion Health is typically responding to 20 or so tenders globally at any point in time with a total value of $500m or more.
Next, there is the sensitive issue of the services that regional hospitals should and shouldn’t deliver. All hospitals must provide services such as ED, routine orthopaedics, maternity, general surgery and general medicine.
But there are more complex procedures that are best done in tertiary hospital specialist centres as equipment can be costly and more importantly the outcomes can be much better.
For example, expensive Da Vinci robots are supposedly better at doing prostate surgery than human surgeons and, if so, then possibly this surgery should be delivered out of three tertiary facilities, rather than the many hospitals that do this surgery today.
Sensible and VERY careful consideration is also needed regarding services that could be better delivered by private providers. One major benefit of using private-sector capacity is that it frees up space in public hospitals, to clear waiting lists and focus on the more complex cases.
Then, funding models, sensible health regions and hospital sizings also need addressing. These are three massive topics that deserve individual articles and the attention of healthcare giants such as Dame Annette King, Des Gorman, Ian Powell, David Meates and maybe even my friend Rob Campbell.
So, a big to-do list, which I believe will go a long way to getting NZ's $24 billion health service back on track.
There is no need for any more think tanks, consultancy reports, talkfests, or ideological-driven change. We need to act fast as Canterbury did, and we are lucky to have many seasoned healthcare professionals that could assist.
I wish Dr Verrall all the best with these challenges.